What is Manual Lymphatic Drainage (MLD) and how does it help with surgery?
MLD is a gentle and incredibly soothing massage technique that helps direct and move lymphatic flow out of the swollen surgical area into lymph nodes for processing.
We may not give much thought to our lymphatic system but it’s our body’s second circulatory system and it plays an important role in supporting our immune system by detoxifying all the tissues in our body. It is especially important in healing after physical trauma or surgery.
Swelling is an important part of the surgical healing process as the lymphatic system delivers white blood cells and proteins to heal the tissue, but our lymphatic system can actually slow down or even complicate wound healing when it’s overwhelmed by surgery or trauma or congested by unhealthy living. A healthy lymphatic system before, during, and after surgery helps facilitate optimal healing.
Used pre and post-surgically, Manual Lymphatic Drainage can accelerate your healing process by helping to move swelling, bruising, debris, toxins, and waste into your lymphatic system where they can be effectively eliminated.
After surgery, your lymphatic system transports white blood and other immune cells to injured tissue and removes swelling and inflammation (including waste, toxins, necrotic tissue, debris, and other harmful substances).
Surgical procedures can disrupt and overwhelm the lymphatic system which can cause excess lymph fluid to accumulate. Excess lymph in or around surgical sites increases inflammation and swelling and actually inhibits the healing process. Accumulated lymph fluid can result in infection, excess scarring, seromas, and fibrosis.
Manual Lymphatic Drainage helps move swelling to its proper lymphatic drainage areas, helping to ensure that waste from the surgical site is effectively removed. Waste from the surgical site is then processed in the lymphatic system and ultimately eliminated through your colon and kidneys.
What Manual Lymphatic Drainage is NOT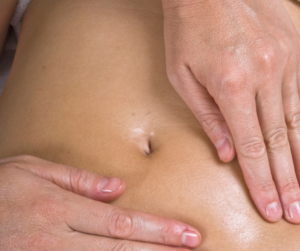
Much of what you see on the internet is not actual Manual Lymphatic Drainage.
MLD is not machines or gadgets. It is not aggressive or deep massage. It is not pushing lymph out of your incisions and it does not hurt at all.
With MLD, I simply assist your lymphatic system in healing your body by moving lymphatic fluid and inflammation into healthy nodes for processing using a gentle, healing touch.
What can I expect with Manual Lymphatic Drainage?
The words massage and drainage actually don’t fit this treatment very well. The superficial lymphatic system lies just under the skin.
To directly affect lymphatic fluid movement I use gentle skin stretching and rhythmic pumping in the direction of the appropriate nodes with pressure as light as the weight of a nickel. Anything stronger goes right through the lymphatic system and into the muscles.
The “drainage” is happening within the lymphatic system as we coax inflammation and debris into the appropriate nodes.
I do NOT open your incisions and no additional external drainage happens during an MLD treatment once your drain ports are removed. Your body takes care of processing all the fluid that we direct to the lymph nodes.
Pre-surgical treatment involves preparing the lymphatic system for optimal healing through a full-body lymphatic massage with a focus on the surgical region.
Post-surgical treatment is tailored to your surgical procedure, and your individual healing needs, and focuses on the surgical region as well as supporting the regional nodes.
You can expect a relaxing and gentle, yet profoundly effective treatment. Many people even fall asleep. I also walk you through home care instructions to help you support your healing in-between visits.
My office is located in a quiet building with very little foot traffic so you are unlikely to encounter anyone on the way to your appointments.
When is Manual Lymphatic Drainage used in the healing process?
MLD is most important during the first 2-3 weeks following surgery. Post-op treatments are scheduled 4 days apart beginning on post-surgical day 4.
Your pre-surgical MLD treatment should be scheduled 5 to 7 days before your surgery (10 to 14 days for a full facelift) to ensure that your lymphatic system is as healthy and prepared for surgery as possible.
How many sessions will I need?
The answer to that depends on the type of surgery you received, how extensive it was, your overall health, and your body’s healing response.
You can not overdo gentle MLD and you will be doing daily home care before and after surgery in addition to your MLD treatments.
MLD is sold in an initial package of 5 treatments with additional appointments added on as needed. We begin with one pre-surgical and 4 post-surgical treatments and then reevaluate your healing in week 3. Most people move to one treatment a week for 3 more weeks (six post-surgical MLD weeks in total).
For breast reconstruction, we work closely to tailor your MLD treatment plan to the various stages of your individual reconstruction and your body’s response to each step of the process. Cancer must be in remission for breast reconstruction MLD.
For tummy tuck, rhinoplasty, blepharoplasty, orthopedic surgeries, mommy makeover, and breast implant or reduction surgery, you should plan for 1 session in the week prior to surgery, two sessions a week during the first 2-3 weeks (roughly every 4 days starting at day 4), then one session a week ongoing for a total of 4-6 weeks.
Scar treatments (which are very different from MLD treatments) can begin for most people at week 6.
For facelift, the post-surgical guidelines above are the same, but I recommend you book your pre-surgical appointment 2 weeks prior to surgery so that you can begin your home massage to establish what we call anastomosis or alternative lymphatic pathways. This is important because your incisions will inhibit normal lymphatic drainage to the nodes in front of and behind the ear.
 With liposuction (including BBL), damage to the lymphatic system from the cannula is more extensive and it can take several weeks to a few months to fully re-establish healthy lymphatic flow.
With liposuction (including BBL), damage to the lymphatic system from the cannula is more extensive and it can take several weeks to a few months to fully re-establish healthy lymphatic flow.
Liposuction involving 2+ regions, or removal of 2+ liters, and lipo plus other surgeries, usually requires more treatments. It takes several weeks to address normal lipo lumps and bumps and help avoid fibrosis with both MLD and myofascial release work.
I recommend one MLD session in the week prior to surgery and then MLD treatment every 4 days in the first 2 weeks. Most people then move to treatments every 6 days in weeks 3 and 4 and then every 9-10 days for MLD plus myofascial release moving forward, depending on how extensive their lipo surgery was and their body’s healing response.
Lumps, bumps, seromas, fibrosis, and scarring
One of the primary goals of early MLD treatment for all surgeries is to assist the body in healing tissue damaged by surgery to help prevent more serious long-term issues like seromas and fibrosis.
Lumps, bumps, and tight-feeling tissue are a normal part of the early healing process, especially after liposuction, as the body clears out necrotic fat cells.
Seromas are encapsulated, trapped, fluid and generally occur about 7 to 10 days after drains are removed (or earlier if drains are disrupted).
The fluid that becomes a seroma can be taken care of by your lymphatic system with MLD and compression before it encapsulates and requires medical intervention.
Fibrosis feels like dense, taught, scar tissue, often in the area where liposuction was performed. Fibrosis is abnormal (yet common) healing involving the overproduction of connective tissue, resulting in bands of scaring through many layers of tissue. It can be painful, unsightly, and can even limit proper movement.
Fibrosis is different than the normal lipo lumps and bumps that you feel during healing. It takes time to develop fibrosis and early MLD and myofascial release work (when appropriate) can help greatly to avoid fibrosis formation.
Both seromas and fibrosis need to be treated as soon as you notice them, the longer you wait the more difficult (but not impossible) they are to treat. First and foremost, please check with your doctor about any concerns.
To reduce the chances of seroma and fibrosis development, follow all your doctor’s orders, take care of your drains, wear your compression exactly as prescribed, and get Manual Lymphatic Drainage to help your body process extra lymphatic fluid during the healing process.
If you didn’t receive MLD immediately after surgery and your doctor has some concerns, don’t despair. Our bodies have an amazing ability to heal with the right assistance.
In addition to being an Advanced Lymphatic Drainage Practitioner, I’m also Certified in the Arvigo Techniques of Maya Abdominal Therapy. I was trained directly by Dr. Rosita Arvigo in the US and Belize. I’ve successfully helped many clients with abdominal adhesions, fibrosis, and range of motion limiting scarring over the years.
What’s my investment and when should I schedule? 
To facilitate optimal healing, MLD is available in an initial package of 5 visits for $450. Additional appointments are $90. Pre-booking a package ensures space on my calendar and saves you $50.
I have a busy schedule and can only guarantee space on my calendar if you pre-book prior to your surgery. Please contact me to schedule as soon as you have your surgery date.
If you are post-surgery and did not pre-schedule a MLD package, but now realize that you urgently need MLD, please reach out to me and I will try to get you scheduled for a treatment to reduce chances of healing complications. Non-package MLD intake appointments are $140 and follow up appointments are $95.
I look forward to partnering with you on your healing journey!
Selected references and further reading about MLD and surgical recovery:
Summary from https://www.massagemag.com/manual-lymph-drainage-benefits-cosmetic-surgery-patients-12794/
- Bruising reduction. Cells transported by the lymph system are moved away 10 times faster with MLD. Bruises heal in a fraction of the time, allowing clients the ability to resume activities of daily living, without having to wear sunglasses for months to hide bruises.
- Edema reduction. MLD reroutes lymph fluid to collateral and viable pathways untouched by surgery to allow for accelerated drainage, as opposed to the slow trickle of tissue fluids in the operative site.
- Pain management. As pressure of lymph fluid decreases around nerves, pain and discomfort are relieved and require less pain medication.
- Scar-tissue prevention and fibrosis reduction. Lymph fluid left to build up below incisions or sitting in interstitial space can solidify, causing the formation of scar tissue and fibrotic tissue. These tissues are often felt as ball-like substances below the skin surface. MLD prevents lymph fluid build up and solidification, for a seamless scar.
- Infection prevention. Postsurgical MLD is important when considering that stagnating lymph fluid can become infectious material and warrant artificial drain insertion—which is painful, costly and time consuming.
https://www.michellerankin.com/wp-content/uploads/2022/10/Research-Manual-Lymphatic-Drainage-An-integral-Component-of-Postoperative-Care.pdf “Patients who do not undergo postoperative decongestive therapy have a predictable and consistent postoperative course. Patients experience postoperative edema which peaks 2-4 days following surgery and is followed by soft tissue fibrosis of the operated area by day 14-42. The extent of the edema and fibrosis depend on the following variables: 1) the operated location (dependent areas swell more), 2) the patients activity level 3) fluid retention 4) previous surgery on the same area. We see complete resolution of postoperative edema and fibrosis in this group between 9 months to 18 months following surgery. In the ten groups listed above who underwent MLC and Deep Tissue Massage, postoperative swelling and fibrosis resolved within 6 weeks to 3 months, thereby shortening recovery significantly.”
https://pubmed.ncbi.nlm.nih.gov/23810354/ “A significant group effect was observed for active knee flexion, with post hoc tests demonstrating a significantly greater active knee flexion in the MLD group when compared with the control (no MLD) group at the final measure prior to hospital discharge (day 4 postsurgery) and at 6 weeks postsurgery.”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4075221/ “Eighteen women aged between 18 and 60 years participated in this study, in the late PO period following lipoabdominoplasty or liposuction in the abdomen, flanks and lower trunk, which showed tissue fibrosis of the flanks and abdomen regions. They were divided into two groups: Liposuction group and lipoabdominoplasty group. A total of twelve sessions of therapeutic ultrasound followed by the Manual Lymphatic Drainage were performed. The patients were assessed with regard to pain, oedema and tissue fibrosis in different moments: Initial assessment, during assessment and final assessment through the application of the protocol of evaluation of cysts fibrosis levels. There was a statistically significant reduction of pain, swelling and tissue fibrosis in both groups [With MLD and Ultrasound].”
Herrera, J., Henke, C. A., & Bitterman, P. B. (2018). Extracellular matrix as a driver of progressive fibrosis. The Journal of clinical investigation, 128(1), 45–53. https://doi.org/10.1172/JCI93557. Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5749528/
High-definition liposculpture: what are the complications and how to manage them https://www.semanticscholar.org/paper/High-Definition-Liposculpture%3A-What-are-the-and-How-Danilla-Babaitis/d87c0eb879744bccc35e5ee6b6aa16237d8fd85d
Nonoperative treatment of lymphedema https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5891656
Swelling and bruises should be reduced as early as possible and it may start even in the early PO period to prevent fibrosis. Tacani RE, Alegrance FC, Assumpção JD, Gimenes RO. Investigação do encaminhamento médico a tratamentos fisioterapêuticos de pacientes submetidos a lipoaspiração. O Mundo da Saúde. 2005;29:192–8.
Comparison of Manual Lymph Drainage Therapy and Connective Tissue Massage inWomen With Fibromyalgia: A Randomized Controlled Trial https://www.sciencedirect.com/science/article/abs/pii/S0161475408003527
Facelift and Patterns of Lymphatic Drainage: https://academic.oup.com/asj/article/32/1/39/210354
Compilation of resources: https://www.sciencedirect.com/topics/medicine-and-dentistry/manual-lymphatic-drainage

