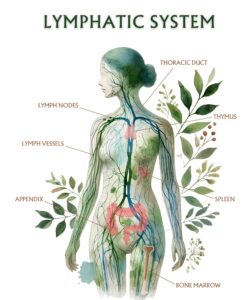
Lymphedema is a chronic condition caused by lymphatic system damage or insufficiency. It is common following cancer treatment, especially after lymph node removal or radiation. It can also result from trauma, infection, or be congenital. The swelling occurs when lymph fluid accumulates in tissues, leading to discomfort, reduced function, and progressive tissue changes if untreated.
Our clinic provides targeted manual therapy within a Complete Decongestive Therapy (CDT) framework—the gold standard for managing lymphedema. CDT includes Manual Lymphatic Drainage (MLD), compression therapy, movement, and skin care.
What Is Complete Decongestive Therapy (CDT)?
CDT is a two-phase medical approach that reduces fluid buildup and fibrosis and maintains those gains through structured home care. This protocol is widely supported in both clinical research and oncology guidelines.
Phase I – Intensive Reduction Phase
- Manual Lymphatic Drainage (MLD): A gentle, skin-stretching technique that reroutes fluid into healthy lymphatic channels
- Compression Bandaging: Low-stretch wraps help prevent reaccumulation of fluid and improve muscle pump function
- Fibrosis Reduction: Manual techniques to break down thickened tissue and improve skin mobility
- Therapeutic Movement: Gentle, guided exercise to promote lymphatic return
- Skin and Nail Care: Preventative care to reduce infection risk, especially cellulitis
Phase II – Maintenance Phase
- Compression Garments: Custom-fitted sleeves, stockings, or wraps to maintain limb volume
- Self-Manual Lymphatic Drainage: Patient-led maintenance techniques taught by a therapist
- Home Exercise: Continuation of low-load movements to maintain lymph flow
- Monitoring: Ongoing tracking of swelling, tissue changes, and functional impact
This multi-phase treatment model has been shown to significantly reduce limb volume and improve quality of life. A systematic review by Oremus et al. (2012) found that CDT reduces lymphedema volume by 30–60% in many patients. In a prospective trial, Moseley et al. (2007) observed that patients who completed Phase I followed by a structured maintenance plan had significantly lower rates of recurrence.
How Lymphedema Affects the Body 
Left unmanaged, lymphedema can create a cascade of complications:
- Progressive swelling of one or more limbs, sometimes involving the trunk, face, or genitals
- Pain, heaviness, or reduced mobility
- Fibrotic tissue changes, skin hardening, or “woody” feel
- Recurrent skin infections such as cellulitis
- Postural changes and compensatory movement patterns
- Emotional and psychosocial impact
While swelling may appear mild at first, early treatment reduces the risk of long-term disability and irreversible tissue changes.
Manual Therapy Goals in CDT
Our massage therapists are trained in MLD techniques to support fluid movement and tissue softening. Manual therapy may:
- Improve regional lymph drainage through healthy lymphatic watersheds
- Reduce fibrotic tissue and improve fascial mobility
- Ease heaviness, tightness, or pain caused by fluid buildup
- Support better posture and range of motion
- Reinforce self-care techniques that prevent flare-ups
A randomized trial by Johansson et al. (1999) showed that MLD combined with compression led to significantly better outcomes than compression alone in women with postmastectomy lymphedema. Similarly, Szuba et al. (2002) found significant improvements in limb volume, pain, and function when MLD was used as part of CDT.
Clinical Considerations
MLD is a low-pressure, non-invasive technique. It is generally well tolerated but contraindicated in patients with:
- Active infection or fever (e.g., cellulitis)
- Acute congestive heart failure or decompensated renal failure
- Deep vein thrombosis (DVT)
- Malignancy without medical clearance
We will review your full medical history before starting treatment.
Common Indications for Lymphedema Massage
Our therapists provide targeted care for:
- Post-mastectomy and chest wall lymphedema
- Post-radiation fibrosis or lymphatic congestion
- Upper extremity swelling after axillary node dissection
- Pelvic, leg, or genital swelling after gynecological or prostate cancer
- Head and neck lymphedema after skin, thyroid, or throat cancer
- Post-infectious lymphedema (e.g., cellulitis or filariasis)
- Primary (congenital) or idiopathic lymphedema
Sessions are tailored to stage, location, and fibrosis level. We collaborate with oncology teams and lymphedema therapists when compression fitting or advanced monitoring is needed.
